 The author applies his experience designing ankle foot orthoses to propose that, instead of using diagnostic language to describe medial column ligamentous failure, practitioners learn a new, descriptive language to understand the nature of a patient’s pathology. Beyond that, he proposes causality due to ligament failure.
The author applies his experience designing ankle foot orthoses to propose that, instead of using diagnostic language to describe medial column ligamentous failure, practitioners learn a new, descriptive language to understand the nature of a patient’s pathology. Beyond that, he proposes causality due to ligament failure.
By Ian Engelman, MS, CPO
Have you read Outliers: The Story of Success by Malcolm Gladwell? In the book, he observes that expertise is developed through tenacity and repeated observation and presents examples of what he calls the “10,000-hour rule” for mastering a craft or field of inquiry.1
I mention this because, over the past 15 years, I have designed more than 15,000 ankle–foot orthoses by working with 3-dimensional plaster models. Each model takes, on average, 1 hour to make—causing some practitioners to burn out. I have remained in the plaster room, however, and, although I don’t pretend to compare myself to the leaders described in Outliers, I have put in my time and therefore have insights to share.
In this article, I present a perspective on, and a theory of, medial column breakdown (ie, ligamentous failure), based on observation and experience, in the hope that data and statistical analysis will follow. Using CubeVue software to process imaging acquired by the pedCAT ultra-low dose computed tomography system (both products of Curvebeam, Warrington, Penn.), I believe that scientific analysis of these injuries is possible through repeatable quantification—perhaps for the first time.
A few words about the language we speak
The interaction between thought and language is well studied. A linguist can explain how language can limit our thoughts and understanding: Sometimes, it takes a new language and a new tool to break through these limitations. Three-dimensional rendering thus reveals shortcomings of previous 2-dimensional analyses and leads to new definitions.
The old language can restrain perspective and lead us in the wrong direction—here, in part, as a result of using words that describe medial column ligamentous failure in a diagnostic fashion. Look at the following listing; which word or terms do you use to describe this common pathology: Medial instability? Ligamentous laxity? Or adult-acquired flat foot, hypermobility of the first ray, excessive pronation, fallen or collapsed arches, internal rotary dysfunction, posterior tibial tendon dysfunction (stages 1-4), posterior tibial tendonitis, equinus, pes planus, equinovarus, pes planovalgus, or midfoot collapse?
Orthopedists, podiatrists, orthotists, physical therapists, and others might use slightly or substantially different words or terms, but each language imposes limitations on understanding.

Perspectives on ‘medial column breakdown’
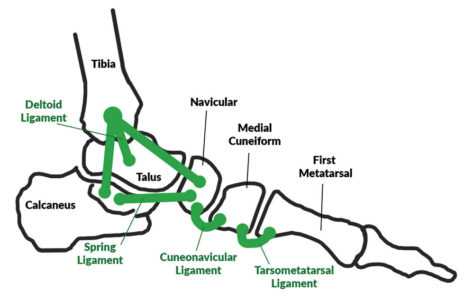
Different professions have their own view of the pathology that I propose we generically call medial column breakdown (Figure 1).
Orthopedic surgery. Two common terms are hypermobility of the first ray and adult acquired flat foot. In addition, pathology is discussed in terms of stages (1, 2 ,3, and 4). True, the degree of medial column breakdown can vary, but the language of stages is little more than a subjective label of the degree of deformity, saying nothing about the location of the failure or the type of pathology of the foot—for example, failing to speak to hind-foot or midfoot participation.
For me, hypermobility of the first ray is an odd way of looking at a failure that is somewhere along the medial column. I agree, however, that there would be increased relative collapse as a secondary effect of greater-than-normal mobility of the first ray. After all, the first ray is a substantially weight-bearing element.
Podiatry. “Posterior tib” is the shorthand I hear most often. This catch-all seems to mean posterior tibial tendonitis or posterior tibial tendon dysfunction. The words lead the mind to think that the causality is weakness of this particular tendon/muscle, and that this one muscle suspends the whole medial column!
That view seems incomplete. Although there can be pain around the posterior aspect of the medial malleolus, such cases are (in my experience) in the minority. Moreover, it seems unlikely that muscles are responsible for the structural stability of the medial column. The human body naturally finds ways to save energy, and firing muscles to keep the medial column from collapsing is an inefficient use of the body’s resources.
Orthotics and prosthetics. In school, pes planovalgus is taught. True, medial column breakdown often has hind-foot valgus, but not in every case. Another favorite closed kinetic-chain description is internal rotary deformity. For some of these cases, there is no obvious tibial internal rotation, yet there are features such as forefoot abduction and hind-foot valgus. In short, it seems clear that not all of these cases present with tibial rotation, and that those that do might not present with the complete set of corresponding deformities.
Physical therapy. Flat foot, pronation, and midfoot collapse are commonly used. These are generic descriptions readily understood by the professional and nonprofessional alike. The terms are useful in a general sense, but have limitations in that they suggest that the “whole” foot has failed.
Stating the organizing principle
Better and more specific terms lead to better, more specific understanding of the origin of the pathological condition. Efforts to describe the mechanisms of the foot and ankle joints often lead to comparisons with everyday articulated elements. I’ve heard these mechanisms described as a hinge, a set of hinges, a sling, a kinetic chain, a mechanical bridge, a 3-legged stool—even a gyroscope! Such comparisons might be helpful to some, but I see no point. Why compare? Instead, I believe we have the capacity to think directly about the bony segments with articular surfaces connected by ligaments.
In the spirit of looking at the medial column pathology in a new way, and for this exercise of experimenting with new language, put aside the old terms and consider a set of more refined, specific terms that connect the categories of medial column breakdown with failure in a specific ligament. The primary assumption is that the architecture of the medial column of the foot is primarily held in position by ligaments that connect bones (Figure 2). Proximally to distally, the major ligaments involved are the deltoid, spring, cuneonavicular, and tarsometatarsal. Again proximally to distally, the bones are the tibia, talus, navicular, cuneiform, and metatarsal.
I propose that failures of these ligaments are the primary contributors to medial column breakdown, but are by no means the only structural connections. It is also possible that breakdown of the lateral column will affect the shape of the foot and lead to a condition that mimics medial column breakdown.
Three-dimensional analysis
New tools enabled by 3-dimensional rendering provide the possibility of a paradigm shift in understanding the interactions of bones with their articular surfaces. The most advanced system available is PedCAT, described earlier. The technology of this imaging system is superior to others for a profoundly important reason: The image is taken during weight bearing. This is critical for practitioners who want to understand and to help people walk, because ambulation is, after all, a weight bearing activity.
Information about the relationships among the bones of a hanging foot, for example, is not particularly helpful; this forces the practitioner to guess how those bones might line up during weight bearing. More profound analysis is the ability to scan in real-life conditions.
The foot will present in one way on a flat surface and slightly differently in the curved condition of a shoe. Currently, there is a habit of scanning on a flat surface. Evaluation during single-limb weight bearing in a shoe, with a foot orthotic, or inside an ankle foot orthosis would be the most relevant. Even better would be to somehow mimic the increased forces produced in ambulation. For now, however, these 3-dimensional scans are so profoundly better than 2-dimensional radiographs that, first, they are redefining all the metrics and, second, important new parameters are being, and will continue to be, created.
Many validation possibilities could lead to quantification and efficacy of treatment. For now, I’ll keep the focus on a better understanding of medial column breakdown by looking closely at where the failure might be.
The word “failure” is used in this article, but any of the following possible ligamentous conditions could be substituted: stretched, attenuated, degenerated, partial tear, complete rupture, or a combination of any of these. In examining more than 15,000 plaster models, I’ve noticed shapes/pathologies that repeat themselves. These are pathologies that are not well explained by the old language, and they seem to fall into distinguishable categories.
New words to describe categories of pathology
Using CurveBeam technology, it is possible to manipulate images to strip away (virtually) muscle and soft tissue from a sample from each category. With careful examination, it becomes apparent where the failure is likely to be. From its location, we can pinpoint a suspicious ligament.
The exercise of distinguishing categories forces one to label those categories. I’ve created 5 labels and their corresponding ligament (plus 1 label for the normal foot):
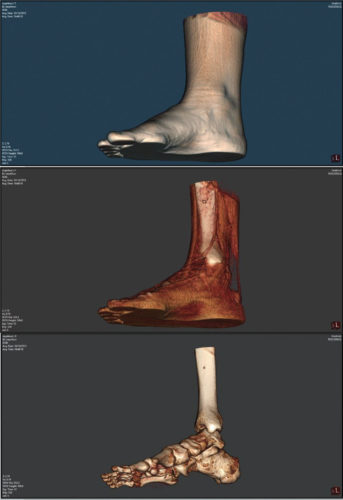
Normal foot (no ligamentous problems). Space limitations prevent me from showing all the angles and internal alignments of a normal foot. I present it here (Figure 3) because, if we are going to investigate pathologies, we first have to agree on what a normal foot is:
- From the sagittal view of the medial column, a relatively straight line originates from the center line of the talus and runs through the navicular, medial cuneiform, and the shaft of the first metatarsal to the first metatarsal head.
- From the coronal view, the weight line from the center line of the tibia drives straight through the talus, and the calcaneus is substantially underneath.
Next, starting proximally and working distally:
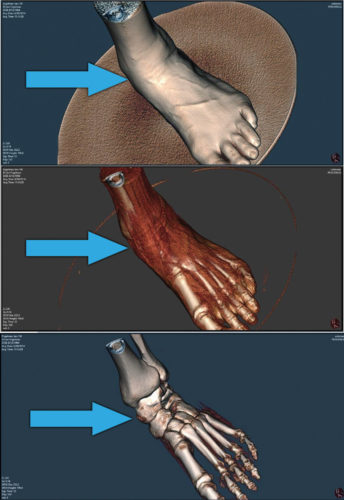
Lateral foot dislocation (deltoid ligament failure). Weakness in the deltoid ligament presents with a foot shape that looks like the foot is dislocated laterally from the weight line (Figure 4). The triangular shape of the deltoid ligament connects the tibia to 3 tarsal bones individually: the calcaneous, the talus, and the navicular. In cases like these, alignment of the medial column can be healthy, but there is increased demand on it structurally because the lateral column is no longer weight bearing. Valgus of the hind-foot is a feature in this category, but forefoot abduction may not present.
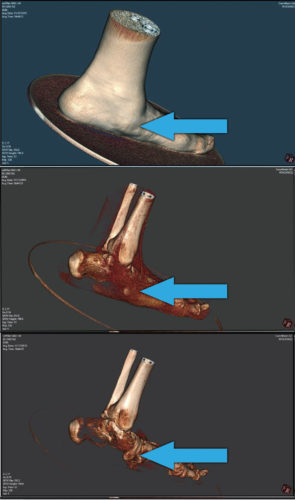
Talar escape (spring [plantar calcaneonavicular] ligament failure). The spring ligament connects the calcaneus to the navicular in a way that holds in the talar head. If this is stretched, the resulting opening becomes large enough for the head of the talus to emerge (Figure 5). This deformity is easy to identify because there is a bony protrusion that is closer (approximately 3 cm) to the medial malleolus than the navicular (approximately 5 cm). With this weakness, the talus rotates inward along with the ankle mortise. Hind-foot valgus and forefoot abduction often result.
Mid-column breakdown (plantar cuneonavicular ligamentous failure). This category seems to be the most common type of medial column breakdown. The ligament that connects the medial cuneiform and the navicular is likely compromised. It’s hard to show in these 2-dimensional images (Figure 6) but, with 3-dimensional rendering and careful rotation, you can see gapping between these 2 tarsals. The declination of the talus points through the navicular but not to the cuneiform. It’s as if the linear line of segments breaks at an upward angle from which the rest of the bones align on a new straight line directed to the first metatarsal head.
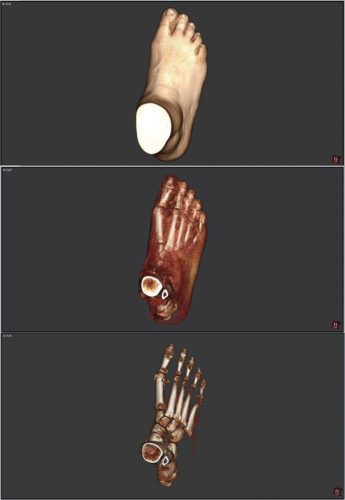
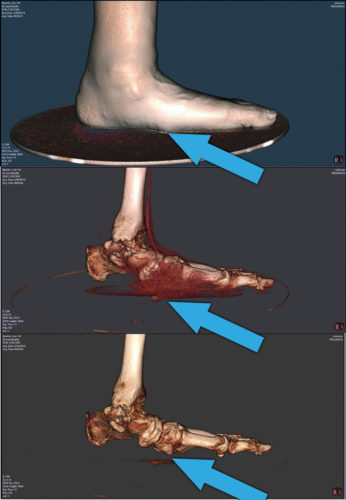
Lisfranc breakdown (plantar tarsometatarsal ligamentous failure). This pathology is noticeably different than the others. The plantar ligament that connects the medial cuneiform to the first metatarsal is damaged (Figure 7). These 2 bones are relatively bulbous and leave an unmistakable bulge on the plantar surface. It is interesting that there is often tolerable weight bearing here, and that the foot can develop a fat pad not unlike the one under the calcaneus. Alignment and stability proximal to the “break” can be in the normal range.
Lateral column flat foot (long [and short] plantar ligamentous failure). This condition does not seem to be a failure of the medial column at all. When the foot is examined, we see good, healthy alignment of the medial column from sagittal and transverse viewpoints. In the coronal plane, the talocrural joint lines up over the calcaneus in a stable way. On examination however, there is undeniable flatness (Figure 8). Perhaps the ligaments supporting the lateral column are compromised in these cases (long and short plantar). In my experience, there are few functional issues from the reports of patients whose foot presents this way.
About imaging
Severe limitations exist in communicating and distinguishing the categories reviewed in this article because we have only words and 2-dimensional images. The experience of 3-dimensional shapes rotating in space affords a deeper understanding of the pathologies. CubeVue software can strip away soft tissue (because it is less dense) to reveal bony substructure. Pulsating between the exterior shape and the interior architecture allows the user to fix their eye on (for example) a prominence and confirm internal anatomy.
Videos available at www.medialcolumnbreakdown.com attempt to show the power of this new technology. I say “attempts” purposely. The human brain has a direct line communication with the hands. Ideally, we would have life-sized models in our hands so that each of us could rotate and examine them simultaneously. This ideal method of communication puts the brain in a more active state and allows even more comprehension. Close approximation is achieved by a first-hand user of Curvebeam with Cubevue: The user with a mouse in hand can volitionally rotate an image in space.
For now, without having the Cubevue program in your hand, watching someone else rotate the object is the best we can do. A picture is worth a thousand words; so, what is a video worth? Here is a best-to-worst list of communication modalities:
- text/words
- picture
- video of a 3D-rendered image, rotated
- 3D-rendered image, volitionally rotated by the viewer
- 3D physical model in hand.
In conclusion
In my view, the ultimate analytical endpoint is a segmented model construct produced by a program like SolidWorks (Dassault Systèmes, Waltham, Mass.) that has virtual embodiments with the exact properties and shapes of bones and ligaments. Such a model would allow any theory to be tested using computer-generated forces. Vectors could be applied with changes in magnitude and direction that mimic stance phase. Computer analysis of emergent pathologies could be modeled by observation of the results that emerge from a virtual weakening of specific ligaments.
Hoping to move the field in that direction, I’ve developed a theory that is based on common sense and insights from my experience.
The concept of distinguishing categories is an academic exercise that helps us understand the root cause of the types of medial column breakdown that we see in our practices. I’ve made a point here of finding examples that highlight and demonstrate failure of a specific ligament; I am not suggesting that all pathological feet be pigeonholed in one of these descriptions. When evaluating a foot with medial column breakdown, I find it useful to keep these distinguishing categories in mind. In many cases, there seems to be a primary ligament and a corresponding shape involved in the pathology; in some cases, it is a combination of two or more failures.
I conclude with four ideas:
- The goal of the practitioner should be to have a deep understanding of the problem at hand. That deep understanding that makes the best solutions possible.
- Instead of using diagnostic language to describe medial column breakdown, I propose a new language that is descriptive.
- The architecture of the foot is primarily due to the ligaments, not the tendons.
- There is an important paradigm shift happening that vastly improves our understanding of these pathologies when we move from 2-dimensional radiographs to 3-dimensional rendering.
Reference: Gladwell M. Outliers: the story of success. Boston, Mass.: Little, Brown and Company; 2008.”
Ian Engelman, MS, CPO, developer of the patented Blaze MI AFO for medial column breakdown, is owner and president of Insightful Products, LLC. He also developed the Step-Smart Brace for drop foot and the Funnel shoe horn.
Figure sources: Figures 1 and 2 supplied by the author. Figures 3-8 supplied by the author using CubeVue software (Curvebeam).
Disclosure: Insightful and Curvebeam collaborate to advance understanding of foot and ankle biomechanics. Neither Insightful Products nor Ian Engleman have any financial relationship with Curvebeam.









I have long believed of the value of the Ped-Cat 3 D CAT scan.
Your article is well presented but I question that since ligaments that are stretched, torn, ruptured in the foot are often a surgical dilemma and do not respond well to non-operative care, what treatments do you associate with your diagnoses?
That makes total sense, thank you Ian. I enjoyed watching your well structured argument on the you tube video as well.
Great job!