www.istockphoto.com #2371089
Although lymphedema in the past has often been overlooked or misdiagnosed, a growing number of certified practitioners are using the conservative treatment techniques of manual lymph drainage and complete decongestive therapy to effectively treat lymphedema patients.
By Harold Merriman, PT, PhD, CLT
The clinical importance of lymphatic system disorders is becoming better known among members of the medical community, including physicians and therapists. Most prominent of these disorders is lymphedema, which involves a buildup of protein-rich lymph fluid in the interstitium.
Some of the most common known causes of lower extremity lymphedema include pelvic or lower extremity cancer and cancer treatment (e.g, lymph node resection or radiation) that can damage the lymphatic system. Other causes of lymphedema may be much more subtle, such as an insect bite or sunburn that could irreversibly damage an already compromised and susceptible lymphatic system. Though lymphedema can be found in all types of individuals, active and fit individuals are less likely than obese individuals to develop lymphedema.
Once the diagnosis of lymphedema has been made, appropriate conservative treatment should be administered. Currently, a certified lymphedema therapist (CLT) is the provider of choice to administer the recommended conservative treatment. Before the 1980s, most of the research and treatment of lymphedema and related disorders occurred in Europe. Now there are also many opportunities for practitioners to obtain advanced training in lymphedema in North America. For example, in North America a number of lymphedema schools teach certification courses that allow practicing clinicians to become certified lymphedema therapists. The Lymphology Association of North America (LANA) administers a nationally recognized lymphedema certification exam to qualified and experienced lymphedema clinicians.1
Though the topic of lymphedema and related disorders is becoming better understood, patients with these disorders may still be ignored, misdiagnosed, or simply unable to find proper treatment. Unfortunately, in many areas of the United States there is a currently a shortage or absence of qualified clinicians who can successfully treat these conditions. This article will briefly review the anatomy and physiology of the lymphatic system and discuss the conservative treatment options for the lymphedema patient.2-5
Lymphatic anatomy and physiology

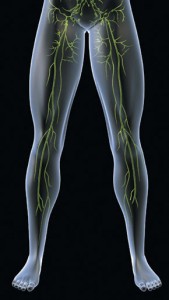
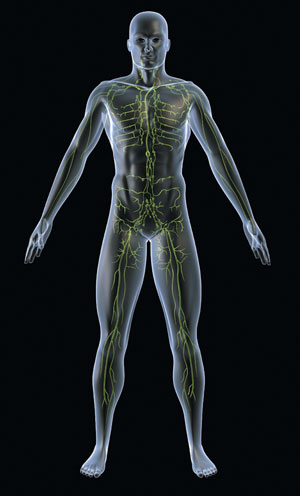
The lymphatic system - www.istockphoto.com #2371089
Lymph originates from blood plasma that leaves the blood capillaries and enters into the interstitum. A percentage of that interstitial fluid then enters the lymphatic system, where it is then called lymph. Lymph matter consists of proteins, water, fatty acids, and cellular components. The typical lymphatic system vessel has a three-layer wall structure and presence of valves, similar to the vessels of the venous system. The inner layer (intima) consists of endothelial cells, the middle layer (media) is made up of smooth muscle, and the outer layer (adventitia) is formed by collagen fibers that are loosely anchored to the extravascular connective tissue.4
The functional unit of the lymph vessel is the lymphangion, which consists of a lymph vessel bordered by two valves. As the lymphangion contracts due to the presence of smooth muscle in the middle layer, the valves provide directionality so that the lymph flows in only one direction. It should be stressed that the lymphatic vessel, unlike the vein, regularly contracts (under the control of the autonomic nervous system) and that this contraction rate can change depending on a number of factors. For example, the lymphangion contraction rate can be stimulated to increase during the hands-on portion of conservative treatment.
While the lymphangions have a distinct three-layer wall construction with valves, not all lymphatic vessels are that well organized. The first type of vessel that collects what will later become lymph fluid is called the initial lymph vessel or lymph capillary. These vessels are blind or dead-end sacs (tubes) consisting of a single layer of endothelium with junctions that can open and close to let in interstitial fluid. The initial lymph vessels lack valves and are located near the blood capillaries. As this fluid flows unidirectionally toward the heart, the lymphatic vessels become larger in diameter and more organized. The lymph collectors and the even larger lymph trunks have the distinct three-layer wall construction with valves. The diameter of the lymph collectors can be as large as 0.6 mm, and the lymph collectors’ valves are spaced 0.6 cm to 2.0 cm apart.3,5 Lymph then flows into the larger lymphatic trunks. The most important lymphatic trunks are the right lymphatic duct and the thoracic duct, which drain the lymph into the venous system near the heart at the right and left venous angles, respectively. The right lymphatic duct drains the right arm, right side of the head, and right upper trunk; meanwhile, the body’s largest lymphatic trunk, the thoracic duct, drains the left arm, left side of the head, both legs, and the rest of the trunk. 2-5
As the lymph moves unidirectionally in the lymphatic vessels, lymph nodes filter and concentrate the lymph and also provide immune surveillance using T & B lymphocytes. The 600 to 700 lymph nodes found in the human body are concentrated in the neck, axilla, chest, abdomen and—most importantly for the lower extremity practitioner—in the groin. In addition to immune defense, the lymphatic system plays a critical role in fluid homeostasis as well as transport and drainage of excess fluids, proteins, and cellular debris from the interstitial spaces that are not reabsorbed by the venous system. One can think of the lymphatic system as the body’s “sanitation system,” whose purpose is to dispose the body’s “waste material.”2-5
Lymphedema results from mechanical failure of the lymphatic system, which leads to an accumulation of protein-rich edema in the interstitium. Mechanical failure means that the “lymphatic load” (amount of lymph transported in a given time period) exceeds what an impaired lymphatic system can handle (transport capacity). In most cases, lymphedema will present itself in a single extremity, or in bilateral cases one extremity will often be more involved than the other (asymmetry). Though one might picture lymphedema occurring mostly in the upper extremity, often lymphedema (especially primary lymphedema) occurs in the lower extremity as well. 2-5
Diagnosis of lymphedema
Lymphedema is the most common disease of the lymphatic system. It is estimated that lymphedema affects 140 million to 250 million people worldwide and at least 3 million Americans.5 Lymphedema exists in two different forms, primary and secondary. Primary lymphedema is believed to result from an abnormally developed lymphatic system that can present either at birth or later in life. In many cases there is no known cause of primary lymphedema. However, in some cases heat, puberty, pregnancy or minor trauma such as insect bites, infections, sprains or strains may be identified. 2-5
In contrast, secondary lymphedema results from a known insult to the lymphatic system that causes a reduced transport capacity. Specific insults to the lymphatic system include surgery, radiation, trauma, tumor growth, infection, and chronic venous insufficiency. 2-5 The two worldwide most common causes of secondary lymphedema are breast cancer surgery and lymphatic filariasis. It should be stressed that even with the advent of less invasive modern surgical techniques such as sentinel lymph node biopsy and lumpectomy, lymphedema may still occur after breast cancer surgery and treatment. 2-5
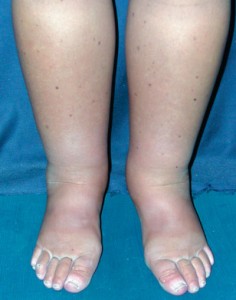
Since lymphedema usually begins distally, it will first be noticed in the lower extremity in the toes, feet, and ankles before progressing proximally up into the thighs. Lower extremity lymphedema would typically be caused by a lymphatic insult in the lower extremity and/or pelvic region, but not by an upper-body lymphatic insult such as breast cancer surgery. The classic sign of lymphedema is a positive Stemmer skin fold sign, which can be defined as a thickened skin fold at the base of the second toe such that the tissue cannot be lifted away from the bone.6 A summary of lymphedema clinical features are listed in Table 1. Since there is no pain associated with lymphedema, the classic symptom that brings a patient to a lower extremity practitioner is edema or infection (cellulitis), which becomes more prevalent as lymphedema severity increases.2,4
It should also be mentioned that combination forms such as lipo-lymphedema are not uncommon. Lipo-lymphedema is a condition in which individuals with lipedema (symmetrical accumulation of fat rather than edema in the subcutaneous tissue) later develop lymphedema in addition to the underlying and ongoing lipedema. Unfortunately, many lipedema patients develop lymphedema since the accumulation of fatty tissue from lipedema causes compression of the superficial lymph vessels.2
Table 1. Lymphedema characteristics
| Clinical Feature | Lymphedema |
| Gender | Women > men |
| Distribution | Unilateral, or bilateral with one leg usually affected more severely (asymmetric) |
| Pain on pressure | Absent |
| Easy bruising of affected area (hematoma) | Absent |
| Distal edema in the foot | Present |
| Stemmer sign | Present (positive) |
Treatment
It is well documented that lymphedema is best treated using conservative methods administered by the certified lymphedema therapist.7-12 Unfortunately at times, lymphedema is still treated with diuretics, which is contrary to treatment guidelines set forth by the International Society of Lymphology and by other lymphedema physician specialists.2,4,12 Perhaps the best known conservative method is manual lymph drainage (MLD) which is a component of complete decongestive therapy (CDT). MLD is a gentle manual treatment technique originally developed in the 1930s by the Danish couple Emil and Estrid Vodder.2,5
CDT consists of two phases; phase I is the treatment phase, and phase II is the self-management phase. CDT and MLD should only be performed after the CLT has determined that no contraindications (e.g., acute infections or cardiac edema) are present. Phase I treatment consists of MLD, compression bandages, exercise (in bandages), and meticulous skin care (to cure/prevent bacterial and fungal infections). Once the reduction in lymphedema begins to plateau, the CLT will transition the patient to the self-management phase II. Phase II consists of compression (typically achieved by a customized garment during the day and bandages at night), exercise (with the limb in either a compression garment or bandages), meticulous skin care, and MLD as needed. Patient compliance with all treatment components (especially during phase II) is the key to a successful long-term outcome, and it is crucial that the patient, therapist, and other caregivers work together as a team.5
One of the most important skills the CLT performs is to provide MLD in the proper sequence. Since MLD increases lymph flow, the therapist does not want this increased lymph flow to overload and further damage an already impaired lymphatic system. For this reason, the CLT may need to initially limit the area to be treated by MLD. For example, if a patient has lymphedema in both legs, then the CLT may elect to initially focus on only one leg. Typically, the lymphedema therapist should first perform MLD on central and uninvolved areas, followed by performing MLD on the involved areas (e.g., the leg). This MLD strategy prepares the uninvolved areas to receive the additional lymph flow from the affected extremity. Again, it is very important that the lymphedema therapist administers MLD in a proper manner and sequence in order to obtain optimal outcomes.5
Proper compression during both phases of CDT is the key to the successful management of the lymphedema patient. If the affected areas do not receive constant and appropriate compression, the improvements achieved by MLD will be temporary (may last only a few hours).5 Therefore, the lymphedema therapist should have a frank discussion with the patient during the initial evaluation outlining the extreme importance of continuous compression of the affected extremity. This discussion should include the reasons why compression is so important, determining the method by which the patient (or other caregiver/family member) can don/doff the compression bandages or garment at home, and alerting the patient to the financial implications of proper compression since two compression garments per affected extremity will need to be purchased about every six months.
In order to achieve appropriate compression during phase I, the lymphedema therapist should use textile-elastic short-stretch bandages that provide a high working pressure when the muscles contract (in contrast with long-stretch Ace bandages, which have a low working pressure). These compression bandages should be applied in such a way that there is more compression distally than proximally. This compression gradient can be achieved by applying more layers of bandage distally and fewer layers proximally.
The lymphedema patient is ready to be fitted for a garment (used for phase II) when the improvements in limb circumference measurements begin to “plateau”. Although ready-made lymphedema garments are available, custom garments are usually made for patients with advanced stages of lymphedema. Compression for lower extremities is often in the range of 40 mmHg to 50 mmHg, and values less than 20 mmHg are not suitable for successful lymphedema management.5
Any exercise or activity that contracts the muscles in the affected area will likely benefit the patient, as activity can promote lymphatic system function. However, the patient should be reminded that during both phase I and phase II, exercises of any type or any strenuous activity should only be performed when the affected extremity is compressed by either a bandage or garment. One helpful strategy when developing an exercise program for a lymphedema patient is to start gradually, and to first start with core muscle and breathing exercises, then proceed to more distal exercises, and finally return to the core muscles and breathing exercises. Examples of distal exercises include toe clenches, ankle curls, heel slides and bike riding.5 It is also very important to carefully monitor the affected extremity of the lymphedema patient during and after the exercise and/or activity to determine if the lymphedema has increased, stayed the same or decreased. Of course, if the lymphedema increases, the intensity and frequency of the exercise should be reduced. 5,12
Lymphedema treatment implications
Only a properly trained lymphedema therapist should treat and educate patients with lymphedema. Unfortunately in North America, extensive instruction during physical therapy schooling is not yet standard. The American Physical Therapy Association (APTA), among other groups, is looking for ways to increase the level of expertise among its members. However, with the proliferation of lymphedema certification courses available in North America, many physical therapists and other healthcare professionals are becoming CLTs. These certification courses are 135 hours or more in length and include both didactic and laboratory portions. A number of accelerated certification programs include an extensive pre-course component, allowing the practitioner to take less time off from work. Other important lymphedema resources include the National Lymphedema Network (NLN) and the International Society of Lymphology (ISL).12,13
While lymphedema in the past has often been overlooked or misdiagnosed, a growing number of CLTs are using the conservative treatment techniques of manual lymph drainage and complete decongestive therapy to effectively treat lymphedema patients. An understanding of the pathophysiology of lymphedema on the part of lower extremity practitioners and an ability to recognize the symptoms will enable more patients to get the treatment they need.
Harold Merriman, PT, PhD, CLT, is an assistant professor and General Medicine Coordinator for the DPT Program in the department of health & sport science at the University of Dayton in Dayton, OH.
References:
1. Lymphology Association of North America. www.clt-lana.org (accessed 9/16/2010)
2. Földi E, Földi M, Strößenreuther RHK, Kubik S, eds. Földi’s Textbook of Lymphology for Physicians and Lymphedema Therapists. 2nd ed. Munich: Elsevier, Urban & Fisher; 2006.
3. Kelly DG. A Primer on Lymphedema. Upper Saddle River, NJ: Prentice Hall; 2002.
4. Weissleder H, Schuchhardt C, eds. Lymphedema Diagnosis and Therapy. 4th ed. Essen, Germany: Viavital; 2008.
5. Zuther JE. Lymphedema Management–The Comprehensive Guide for Practitioners. 2nd ed. New York: Thieme; 2009.
6. Stemmer RA. A clinical symptom for the early and differential diagnosis of lymphedema. Vasa 1976;5(3):261-262.
7. Boris M, Weindorf S, Lasinski B. Persistence of lymphedema reduction after noninvasive complex lymphedema therapy. Oncology 1997;11(1):99-109.
8. Casley-Smith JR, Boris M, Weindorf S, Lasinski B. Treatment for lymphedema of the arm–the Casley-Smith method: a noninvasive method produces continued reduction. Cancer 1998;83(12 Suppl Am):2843-2860.
9. Földi E, Földi M, Clodius L. The lymphedema chaos: a lancet. Ann Plast Surg 1989;22(6):505-515.
10. Földi E. Treatment of lymphedema and patient rehabilitation. Anticancer Res 1998;18(3C):2211-2212.
11. Ko DS, Lerner R, Klose G, Cosimi AB. Effective treatment of lymphedema of the extremities. Arch Surg 1998;133(4):452-458.
12. International Society of Lymphology. The diagnosis and treatment of peripheral lymphedema. 2009 Consensus Document of the International Society of Lymphology. Lymphology 2009;42(2):51-60.
13. National Lymphedema Network. www.lymphnet.org (accessed 9/16/2010)








Excellent discussion!! Thank you.
Excellent article!
what could be the differential diagnosis when chronic disabling pain is present?