By Christina Hall Nettles
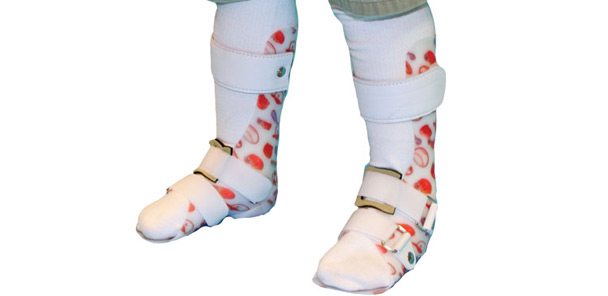
Finding shoes that fit over ankle foot orthoses (AFOs) is a challenge for thousands of children with neuromuscular disorders that affect walking ability. Parents have waited patiently while custom AFOs were molded and fitted, only to find themselves at wit’s end when trying to finish the morning dress routine. Clinicians may become equally frustrated when their young patients’ functional mobility is thwarted because their shoes compete with the goals of a carefully designed orthotic device.
Brent Johnson, CPed, a pedorthist in Toronto, applied his engineering expertise to the problem of finding a footwear-AFO combination that would help his son, Jacob, who has cerebral palsy (CP), better ambulate.
“When he was younger, our son was close to walking because he could stand from a kneeling position or scoot along furniture. Traditional AFOs and the shoes that fit over them improved his standing ability but took away his independent mobility, because their size and nature required someone else to transition him into an upright stance,” Johnson said.
Johnson hybridized a custom orthotic device in a sophisticated supple leather boot that allowed flexibility for gait transition and support while standing, but the product was not reimbursed by traditional insurance plans and was discontinued.
Shoes that are specially designed to accommodate AFOs are commercially available, but many patients and practitioners are not aware of this option. Orthotists typically recommend wearing closed-toe, low-heeled shoes over AFOs to protect the foot and facilitate lever-arm action at heel strike. Wearing too-small shoes puts children at risk for skin lesions and may compromise alignment or gait, and emotional and financial strain can skyrocket when they outgrow AFOs and shoes several times a year.
Outside clinical settings, parents in support groups for CP and other disorders report oversized sandals with elongated Velcro straps are easy to don and doff in relation to AFOs, but Robert S. Lin, CPO, national residency director for Hanger Prosthetics and Orthotics in Newington, CT, cautioned against buying flimsy sandals or grossly oversized shoes.
“Shoes that are too long cannot support gait or weight transition,” Lin said. “If the patient’s foot is a size three, try a size four EEE rather than a standard size six to assure the width accommodates the orthosis across the catch point of the metatarsal heads and the toe break is in optimal position for push off and toe extension.”
Katy Monnot blogs about finding shoes, equipment, and therapy for her four-year old son, Charlie, who has CP.
“Specially made shoes were always heavier, which probably means better quality, but when your child already has low muscle tone, that’s an extra burden. My son could barely pick up his legs in specially made shoes and did much better in off-the-rack athletic-type shoes,” she said.
Monnot’s physical therapist recommended pulling out removable insoles from her son’s store-bought shoes to better accommodate AFOs.
“The most frustrating aspect is that you don’t know if a shoe is going to work until after you’ve destroyed it, which means no returns,” she said.
Lin suggested his patients who prefer traditional shoes bring them in unworn so he can evaluate their potential for fitting over an AFO.
If a practice lacks the resources to provide and fit custom-made shoes on site, he recommended clinicians hand out preprinted sheets with names of local stores and online manufacturers that sell shoes in various widths or mixed-size pairs for patients who require an AFO on only one limb. Practitioners should also follow up with these patients after the AFOs have been delivered.
Early in the course of therapy, well-meaning parents may try high-top shoes instead of, or over, a stable AFO.
“Those shoes make a hinged or articulated AFO virtually worthless,” Lin added, noting the importance of making sure parents understand the purpose of AFO and shoe combinations as therapy progresses.
Clinicians are overworked and parents are under financial strain, but taking an extra few minutes at follow-up visits to evaluate gait in new shoes can ensure specific AFOs are enhanced for independent mobility, he emphasized.
“Every quarter-inch of improvement is worth fighting for,” Johnson agreed.
Sponsored by an educational grant from SureStep









My daughter, 6, has Nuerofibromatosis type 1. She has extremely low muscle tone. Her feet are completely flat, so even without her AFOs, she is an extra-wide in shoes. Her ankles look like they are “melted” off her legs, with her inside ankle bone almost touching the ground.
She should be wearing her AFOs every day, all day, but we are lucky if we get 3-4 hrs every other day. There are no shoes that are “girly” & being that Kate has 2 sisters with fun, pretty, hip shoes…. it is awful for her! (and for us – a constant battle to get her to wear her AFOs, because that means she has to wear her “ugly” shoes…).
Many tears, mostly from her, but from me too (as a mom, you want you baby girl to be happy & have fun). It seems silly – she’s in good health & we do count our blessings!!! But for little girls, cute boots, shoes, & flip flops are such a big thing… I never thought that shoe shopping would be such an emotionally charged (& usually tear-driven) event.
I am desperate for any suggestions. I am aware of the happy feet, hatchback ect. options, & have purchased the black mary jane (size 1 1/2 eee wide) shoes. That is what she wears with pants. But now that summer is coming, UGGGG! Help! Kate is such an awesome kid! It breaks my heart & I would love to offer her something that she can wear with confidence & makes her feel happy!!!
Thanks so much!
Cindy Cochran