iStockphoto.com 510537007
As slacklining’s popularity grows, researchers have begun to uncover physiological and neurological evidence for how and why the activity may be beneficial to people with balance, strength, and mobility issues.
By Brigid Elsken Galloway
Dakota Collins sways precariously as he walks along a narrow nylon strap suspended a few feet off the ground. The strap bounces like a trampoline beneath his feet. He sways his arms from side to side and above his head. At any moment you think he might fall, until you realize he isn’t flailing his arms. He is using them to find his balance—and balance has been the impetus behind Collins’ remarkable rehabilitation. This is slacklining.
Watching the agile 23-year-old cross the slackline, you would never guess that he was born with a clubfoot. Collins spent the first four years of his life with his right leg in a cast. His right foot is two sizes smaller than his left, and until he began slacklining, his right leg was also significantly smaller than the left, with less muscle tone. His shoulders tilted from the resulting scoliosis. Although early surgery and medical intervention helped correct his gait, his posture was altered after years of compensation. Slacklining changed that.
“It helps keep my body balanced,” Collins said. “It has done amazing things for me physically, mentally, and spiritually. Now I can’t really tell a difference between my left and my right sides.”
Collins grew up in Fort Collins, CO, spending a lot of time outdoors. He was drawn to slacklining about five years ago and was surprised to discover it was a “legit sport.” For him, it has become a practice (like yoga or meditation) to help improve concentration, balance, and overall physical fitness. Although Collins is now adept at highlining—an extreme version of the sport performed hundreds of feet off the ground—he introduces his students to a much less intimidating version, just a few inches off a tumbling mat.
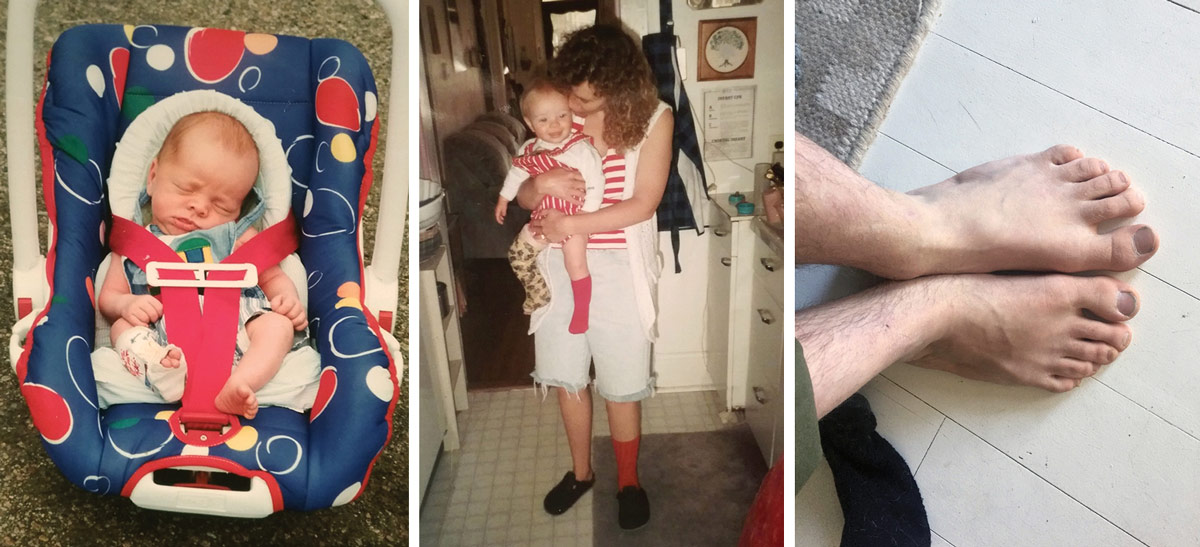
Dakota Collins found that slacklining helped address balance and strength deficits related to his being born with clubfoot (left, center); clubfoot was also responsible for his right foot being two sizes smaller than his left as an adult (right). (Photos courtesy of Dakota Collins.)
As owner of Rocky Mountain Slackline, Collins teaches slackline techniques and travels around the world performing and promoting the sport. He is not a physical therapist, but he shares his experience with school children and physical therapists.
“Keeping my shoulders up and controlling the balance of my arms allowed me to walk better because I was much more aware of my body,” he says. “It changed my need to compensate for my right leg and I was able to build muscle in my right leg.”
Slacklining basics
Although it resembles tightrope walking, the distinction of slacklining is that participants balance on a 2-inch wide, flat nylon strap that’s strung with less tension than a tightrope to give it bounce. The sport is said to have originated in the mid-’80s in California’s Yosemite Valley by climbers who were looking for ways to improve their balance.1 Then, in 2012, Andy Lewis’ slacklining performance at the Super Bowl halftime show (starring Madonna) propelled the activity into the spotlight.2
Slacklines cropped up on college campuses and in parks, predominately for recreation among teens and young adults. Recent slackline festivals have been held in Brazil, Sweden, Turkey, Poland, and France. In the US, Austin, TX; Richmond, VA; Vail, CO; and Spencer, IN, host annual events. Wherever there is open space and two poles, trees, or other anchors, a slackline may be found—and on it, a person who desires to defy, if not gravity, then his or her own sense of balance.
Clinical applications

Collins is now adept at highlining, an extreme version of slacklining. (Photo courtesy of Dakota Collins.)
Only in the past 10 years have researchers begun to uncover physiological and neurological evidence for how and why slacklining may be beneficial to people with balance, strength, and mobility issues.
In 2010, a seminal slackline study3 published by Martin Keller, PhD, a lecturer in the Department of Medicine, Unit Sports Science, at the University of Fribourg in Switzerland, demonstrated that as little as four weeks of slackline training was associated with improved balance in 12 healthy adults.
Before training, no study participants were able to maintain balance on the slackline for 20 seconds. After training two to four times a week, 90 minutes per session, for a total of 10 sessions, they were able to balance unassisted on the slackline for at least 20 seconds, as well as perform a variety of tasks, such as walking the line or catching a ball while balancing on the line. After training, Hoffman reflexes (H-reflexes) were significantly diminished compared with baseline values in the slackline group, and had not changed in the 12-person control group, which did no training.3 Keller and colleagues also found that the participants in the slacklining group demonstrated improvement from baseline in dynamic postural stability, assessed using a device with a multiaxial free-swinging platform.
Although the authors noted that similar improvements have been associated with other forms of balance training,4-7 there were two distinctions. First, unlike traditional balance therapy that relies heavily upon the circumjacent ankle joint, Keller found that slacklining activates muscle groups of the ankle, knee, and hip joints simultaneously. Second, anecdotally, the authors observed that participants found slacklining more enjoyable and motivating than classic balance training.
“What you have with the slackline is the unique ability of the brain to tap into the primary or fundamental balance reaction,” said Philip Gabel, PhD, PT, a research fellow at Griffith University in Queensland, Australia. “That’s something that can’t be achieved in a lot of activities. It’s one of the most mind-blowing areas of potential research and rehabilitation in the last 30 years.”
More than 10 years ago, Gabel used slackline therapy to help world-class Australian surfer Julian Wilson. At that point, slacklining had been recognized as a rehabilitation tool for surfing and skiing, but little formal academic research existed. Gabel decided to change that. He was one of the first to conduct scientific research on the therapeutic benefits of slacklining. He has since authored, co-authored, and contributed to numerous studies on its use for therapeutic purposes among various patient populations.
In 2013, Gabel and colleague Simon Mendoza, PT, at Bern Physical Therapy in Switzerland, created a four-stage, 20-step protocol for slacklining training progression so that it could be used more widely for rehabilitation and injury prevention.8 The progression stipulates beginning with a band suspended only a few centimeters above a soft surface as participants gradually complete a series of simple standing positions, followed by movement on the band.
Gabel and colleagues then studied quadriceps activation in a group of 49 men and women with various knee injuries, including osteoarthritis, injuries to the medial collateral ligament and patellofemoral joint, and postoperative menisectomy.9 The participants completed five separate quadriceps exercises in a clinical setting at a self-perceived effort of a strong to maximal contraction. These exercises included two traditional open-chain exercises, two traditional closed-chain exercises, and Gabel and Mendoza’s composite-chain staged slacklining protocol with the slackline anchored at a length of 3 m and a height of 25 cm. The researchers assessed quadriceps activation after each of the exercise conditions.

iStockphoto.com 180833741
“The distinction is that slacklining is that it is a three-dimensional, composite-chain exercise,” Gabel said. “The slackline is fixed at one end, but it moves in three dimensions. That’s where it’s unique and not just a simple toy. It doesn’t work the same way as most of the balance or rehab tools, like balance boards or bongo boards.”
The study found the slackline activity yielded higher quadriceps activation than the other four activity groups, while the perceived effort during slackline activity was significantly lower. But the body-mind connection that slacklining taps into was more directly explored in subsequent studies with older patients who experienced cognitive impairment due to progressive disorders.
Another 2016 study conducted at the University of Oviedo and the University of A Coruña, both in Spain, found slacklining may be a valid cross-training tool for female basketball players.10
Special populations
More recently, Gabel and colleagues pioneered the use of slacklining as a rehabilitation modality in a clinical setting for stroke. Their 2016 case study11 involved an 87-year-old stroke patient who experienced reduced lower limb muscle activation in her right leg, hypertonia, and concurrent postural deficits. Specifically, she exhibited right lower limb weakness, mildly reduced sensation, and reduced balance and general limb control with tonal changes.
A year after her stroke, the benefits of traditional physical therapy had plateaued. In fact, at this point, the patient had experienced three falls after her mobility began to regress. Enter slackline therapy, consistent with the first two stages of the aforementioned protocol. The patient’s functional status improved within two months and was sustained after six months of therapy. The authors concluded that slacklining’s external stimulations activated global-body responses through innate balance and reflex modulations, in addition to activation of the lower limb muscles and trunk core muscles.11
Likewise, research coauthored by Gabel12 involving individuals with Parkinson disease (PD) suggested that slacklining could be used as a safe and effective means of physical therapy. The study consisted of 20 patients with idiopathic PD, 10 of whom were randomized to perform 12 additional 23-minute balance training sessions using a slackline over six weeks (two sessions per week on nonconsecutive days). The remaining 10 patients formed a control group and followed their usual physical activity routine for the study period.
The sessions included a 10-minute warm-up off the slackline, eight minutes of slackline tasks, and a five-minute cool down. The slackline setup was 300 cm long and 30 cm high. Mats were placed beneath the line for safety. Participants were guided through four training blocks, alternately balancing on the left and right legs and in tandem stance with the right or left leg in front.
Although patients in the slacklining group did not demonstrate significant changes compared with baseline for postural stability, they did demonstrate significant improvements related to freezing of gait and fear of falling.
The slackline therapy was also associated with low levels of self-reported tiredness or fatigue.12
A 2016 study authored by Lars Donath, PhD, a professor in the Department of Sport, Exercise, and Health at the University of Basel in Switzerland, investigated 28 healthy older adults (aged 60 years and older), half of whom were assigned to an intervention group and completed six weeks of slackline training.13 Among the 11 participants whose slackline performance improved, functional magnetic resonance imaging findings suggested increased efficiency of the striatal network during the training period.

Philip Gabel, PhD, PT, and colleagues in Australia have successfully used slacklining techniques to improve balance and function in stroke patients. (Photo courtesy of Philip Gabel, PhD, PT.)
The extent to which improved balance and concentration gained from slackline training transfers to other activities remains unclear.
In a meta-analysis of eight trials and 20 healthy participants of various ages,14 Donath and his colleagues found slackline training primarily revealed meaningful task-specific training effects in balance performance tasks that were closely related to the training content, such as slackline standing time and dynamic standing balance. The analysis also noted that two of the eight studies measured transfer effects to other balance tasks and found limited evidence of transference.
“We were training slackline standing, but we didn’t see other improvements in balance tasks that are more remotely related to slackline standing,” Donath said. “For example, children improved on the slackline and on a wooden balance beam. But they did not improve their standing time on one leg or two legs, or in functional balance tests.”
After performing the meta-analysis, Donath and his colleagues recommended that slacklining should be used as one aspect of a multimodal balance program, rather than the sole form of training.
Training testimonial
While researchers around the world are still exploring the efficacy of slacklining as a therapeutic modality, some practitioners in the US are extolling its immediate and lasting physical effects. Dan Murauski, DO, ABIHM, has read the research and applied it—personally, as well as professionally.
Murauski is medical director at Integrative Wellness Group in Chicago, a member of the Chicago Slackliners Association, and one of the organizers of the annual Breathe Slackline and Discovery Festival in Spencer, IN. He recently had an opportunity to test the benefits of his balance training after having a medial meniscus removed. Murauski believes slacklining’s ability to engage a variety of muscles allowed him to recover more quickly than through traditional physical therapy methods alone.
Murauski noted another distinction: Slacking engages all three systemic components of balance: the eyes, the vestibular system, and proprioception. However, as Murauski experienced after knee surgery, the balance system quickly atrophies if it’s not engaged.
“You don’t move the knee much after surgery, so you lose quad and glute strength and lose stabilizer muscles around the knee itself. Everything atrophies a bit,” he said. “Slacklining helps out the hip stabilizers and muscles that cross your knee joint to help regain stability.”
Prevention potential
Although the preventive effects of slacklining have yet to be scrutinized by researchers, Jim Klopman, inventor and author of a book for consumers on improving balance,15 believes it could help mitigate injury risk in those prone to falls.
Klopman is not a medical practitioner, but he uses the principles of slackline balance training to help athletes from multiple sports disciplines —from golfers to basketball players to skiers— improve their performance. He developed a series of slackline-like devices after discovering the benefits for himself. At their Park City, UT, studio, Klopman and his wife and business partner, Janet Miller (a personal trainer) teach athletes these techniques and also work with people with various mobility issues, including multiple sclerosis.
“We see balance as a software system that is out of tune,” he said. “We live in a world that’s been created to accommodate the least balanced among us.”
Klopman believes slackline training reboots the body’s balance system by challenging it. His devices are used in a gym or clinical setting to provide the challenge found in slacklining in a safe, controlled environment. He also developed a series of foot-strengthening positions; each engaged for two minutes on the right foot and left foot, for a total of a 12-minute routine performed using his slackline-like devices.
“Often in PT we work big muscles and do a little bit of balance work, but what keeps that joint in place are the small control muscles,” Klopman said. “Our balance training dramatically improves the stability of joints because we’re improving the signaling to the joint and the small control muscles around the joint.”
Anecdotally, Klopman reports that the benefits of slackline training can be achieved using his devices. Three years ago, 81-year-old Bud Canady began training on Klopman’s foam balancing block device with the goal of improving his overall balance and stability after a series of falls. A seasoned skier, he also hoped to renew his confidence on the slopes. Canady said he believes integrating the principles of slackline balance training into his everyday movement has helped him prevent falls that could have led to injury.
“As you get older, your balance system doesn’t work as well,” he said. “The slackline work retrains your body to handle shocks, when you are thrown off in some way.”
Clinical research has not been conclusive on the transference of benefit or the lasting effects of slacklining training, but Dakota Collins has a theory about its overarching benefits.
“Because slacklining is a mind-body practice, it helped me become more conscious of how I walk and move off the line,” Collins said. “It became like twenty-four hours a day of physical therapy. Now I don’t even think about it. It’s intuitive to me.”
Brigid Elsken Galloway is a freelance writer in Birmingham, AL.
- Slack Line Tools website. https://www.slackline-tools.com/know-how/history/. Accessed June 7, 2017.
- Longman J. That guy in the toga? Call him a slackliner. New York Times website. http://www.nytimes.com/2012/02/07/sports/football/super-bowl-slacklining-gains-stage-in-madonnas-halftime-show.html. Published Feb 6, 2012. Accessed June 7, 2017.
- Keller M, Pfusterschmied J, Buchecker M, et a Improved postural control after slackline training is accompanied by reduced H-reflexes. Scand J Med Sci Sports 2012;22(4):471-477.
- Granacher U, Gollhofer A, Strass D. Training induced adaptations in characteristics of postural reflexes in elderly men. Gait Posture 2006;24(4):459-466.
- Taube W, Gruber M, Beck S, et al. Cortical and spinal adaptations induced by balance training: correlation between stance stability and corticospinal activation. Acta Physiol 2007;189(4):347-358.
- Gabel CP, Mendoza S. Slacklining for lower extremity rehabilitation and injury prevention. Int J Athl Train Ther 2013;18(4):14-19.
- Santos L, Fernández-Río J, Fernández-García B, et al. Effects of slackline training on postural control, jump performance, and myoelectrical activity in female basketball players. J Strength Cond Res 2016;30(3):653-664.
- Gabel CP, Rando N, Melloh M. Slacklining and stroke: A rehabilitation case study considering balance and lower limb weakness. World J Orthop 2016;7(8):513-518.
- Santos L, Fernandez-Rio J, Winge K, et al. Effects of supervised slackline training on postural instability, freezing of gait, and falls efficacy in people with Parkinson’s disease. Disabil Rehabil 2017;39(16):1573-1580.
- Magon S, Donath L, Gaetano L, et al. Striatal functional connectivity changes following specific balance training elderly people: MRI results of randomized controlled pilot study. Gait Posture 2016;49:334-339.
- Donath L, Roth R, Zahner L, Faude O. Slackline training (balancing over narrow nylon ribbon) and balance performance: a meta-analytical review. Sports Med 2017;47(6):1075-1086.
- Klopman J, Miller J. Balance is power: Improve your body’s balance to perform better, live longer, and look younger. Austin, TX: Lioncrest Publishing; 2016.